Abstract
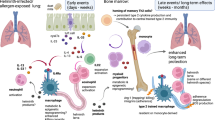
The remarkable increase in asthma prevalence that has occurred over the last two decades is thought to be caused by changes in the environment due to improved hygiene and fewer childhood infections. However, the specific infections that limit T helper type 2 (TH2)-biased inflammation and asthma are not fully known. Infectious organisms, including commensal bacteria in the gastrointestinal tract and hepatitis A virus, may normally induce the development of regulatory T (TR) cells and protective immunity that limit airway inflammation and promote tolerance to respiratory allergens. In the absence of such infections, TH2 cells—which are developmentally related to TR cells—develop instead and coordinate the development of asthmatic inflammation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

C.C

C.C
Similar content being viewed by others
References
Cookson, W. The alliance of genes and environment in asthma and allergy. Nature 402, (Suppl. B) B5–10 (1999).
Van Eerdewegh, P. et al. Association of the ADAM33 gene with asthma and bronchial hyperresponsiveness. Nature (doi:10.1038/nature00878, 10 July 2002).
Fahy, J.V., Corry, D.B. & Boushey, H.A. Airway inflammation and remodeling in asthma. Curr. Opin. Pulm. Med. 6, 15–20 (2000).
von Mutius, E. The environmental predictors of allergic disease. J. Allergy Clin. Immunol. 105, 9–19 (2000).
Strachan, D.P. Hay fever, hygiene, and household size. Brit. Med. J. 299, 1259–1260 (1989).
von Mutius, E. et al. Skin test reactivity and number of siblings. Brit. Med. J. 308, 692–695 (1994).
Ball, T.M. et al. Siblings, day-care attendance, and the risk of asthma and wheezing during childhood. N. Engl. J. Med. 343, 538–543 (2000).
Riedler, J. et al. Exposure to farming in early life and development of asthma and allergy: a cross-sectional survey. Lancet 358, 1129–1133 (2001).
Platts-Mills, T., Vaughan, J., Squillace, S., Woodfolk, J. & Sporik, R. Sensitisation, asthma, and a modified Th2 response in children exposed to cat allergen: a population-based cross-sectional study. Lancet 357, 752–756 (2001).
McKeever, T.M. et al. Early exposure to infections and antibiotics and the incidence of allergic disease: a birth cohort study with the West Midlands General Practice Research Database. J. Allergy Clin. Immunol. 109, 43–50 (2002).
Shirakawa, T., Enomoto, T., Shimazu, S. & Hopkin, J.M. The inverse association between tuberculin responses and atopic disorder. Science 275, 77–79 (1997).
von Hertzen L. et al. Mycobacterium tuberculosis infection and the subsequent development of asthma and allergic conditions. J. Allergy Clin. Immunol. 104, 1211–1214 (1999).
Strannegard, I.L., Larsson, L.O., Wennergren, G. & Strannegard, O. Prevalence of allergy in children in relation to prior BCG vaccination and infection with atypical mycobacteria. Allergy 53, 249–254 (1998).
Lynch, N.R. et al. Relationship between helminthic infection and IgE response in atopic and nonatopic children in a tropical environment. J. Allergy Clin. Immunol. 101, 217–221 (1998).
Gern, J.E. & Busse, W.W. Relationship of viral infections to wheezing illnesses and asthma. Nature Rev. Immunol. 2, 132–138 (2002).
Stein, R.T. et al. Respiratory syncytial virus in early life and risk of wheeze and allergy by age 13 years. Lancet 354, 541–545 (1999).
Bjorksten, B., Naaber, P., Sepp, E. & Mikelsaar, M. The intestinal microflora in allergic Estonian and Swedish 2-year-old children. Clin. Exp. Allergy 29, 342–346 (1999).
Kalliomaki, M. et al. Probiotics in primary prevention of atopic disease: a randomised placebo-controlled trial. Lancet 357, 1076–1079 (2001).
Gehring, U. et al. Exposure to endotoxin decreases the risk of atopic eczema in infancy: a cohort study. J. Allergy Clin. Immunol. 108, 847–854 (2001).
Lorenz, E. et al. Genes other than TLR4 are involved in the response to inhaled LPS. Am. J. Physiol. Lung Cell. Mol. Physiol. 281, (Suppl. 2) L1106–1114 (2001).
Matricardi, P.M. et al. Cross sectional retrospective study of prevalence of atopy among Italian military students with antibodies against hepatitis A virus. Brit. Med. J. 314, 999–1003 (1997).
Matricardi, P. et al. Exposure to foodborne and orofecal microbes versus airborne viruses in relation to atopy and allergic asthma: epidemiological study. Brit. Med. J. 320, 412–417 (2000).
McIntire, J.J. et al. Identification of Tapr (an airway hyperreactivity regulatory locus) and the linked Tim gene family. Nature Immunol. 2, 1109–1116 (2001).
Mosmann, T.R. & Coffman, R.L. Th1 and Th2 cells: different patterns of lymphokine secretion lead to different functional properties. Annu. Rev. Immunol. 7, 145–173 (1989).
Prescott, S.L. et al. Developing patterns of T cell memory to environmental allergens in the first two years of life. Int. Arch. Allergy Immunol. 113, 75–79 (1997).
Abbas, A.K., Murphy, K.M. & Sher, A. Functional diversity of helper T lymphocytes. Nature 383, 787–793 (1996).
Coffman, R.L. et al. The role of helper T cell products in mouse B cell differentiation and isotype regulation. Immunol. Rev. 102, 5–28 (1988).
Iwamoto, I., Nakajima, H., Endo, H. & Yoshida, S. Interferon γ regulates antigen-induced eosinophil recruitment into the mouse airways by inhibiting the infiltration of CD4+ T cells. J. Exp. Med. 177, 573–576 (1993).
Corrigan, C.J. & Kay, A.B. CD4 T-lymphocyte activation in acute severe asthma. Relationship to disease severity and atopic status. Am. Rev. Respir. Dis. 141, 970–977 (1990).
Cembrzynska-Nowak, M., Szklarz, E., Inglot, A.D. & Teodorczyk-Injeyan, J.A. Elevated release of tumor necrosis factor-α and interferon-γ by bronchoalveolar leukocytes from patients with bronchial asthma. Am. Rev. Respir. Dis. 147, 291–295 (1993).
Hansen, G., Berry, G., DeKruyff, R.H. & Umetsu, D.T. Allergen-specific Th1 cells fail to counterbalance Th2 cell-induced airway hyperreactivity but cause severe airway inflammation. J. Clin. Invest. 103, 175–183 (1999).
Lafaille, J.J. et al. Myelin basic protein-specific T helper 2 (Th2) cells cause experimental autoimmune encephalomyelitis in immunodeficient hosts rather than protect them from the disease. J. Exp. Med. 186, 307–312 (1997).
Pakala, S.V., Kurrer, M.O. & Katz, J.D. T helper 2 cells induce acute pancreatitis and diabetes in immune-compromised nonobese diabetic mice. J. Exp. Med. 186, 299–206 (1997).
Genain, C.P. et al. Late complications of immune deviation therapy in a nonhuman primate. Science 274, 2054–2056 (1996).
Seymour, B.W., Gershwin, L.J. & Coffman, R.L. Aerosol-induced immunoglobulin (Ig)-E unresponsiveness to ovalbumin does not require CD8+ or T cell receptor (TCR)-γ/δ+ T cells or interferon (IFN)-γ in a murine model of allergen sensitization. J. Exp. Med. 187, 721–731 (1998).
Tsitoura, D.C., DeKruyff, R.H., Lamb, J.R. & Umetsu, D.T. Intranasal exposure to protein antigen induces immunological tolerance mediated by functionally disabled CD4+ T cells. J. Immunol. 163, 2592–2600 (1999).
Tsitoura, D.C., Blumenthal, R.L., Berry, G., DeKruyff, R.H. & Umetsu, D.T. Mechanisms preventing allergen-induced airways hyperreactivity: Role of immune deviation and tolerance. J. Allergy Clin. Immunol. 106, 239–246 (2000).
Chen, Y., Kuchroo, V.K., Inobe, J., Hafler, D.A. & Weiner, H.L. Regulatory T cell clones induced by oral tolerance: suppression of autoimmune encephalomyelitis. Science 265, 1237–1240 (1994).
Chen, Y. et al. Peripheral deletion of antigen-reactive T cells in oral tolerance. Nature 376, 177–180 (1995).
Hansen, G. et al. CD4+ Th cells engineered to produce latent TGF-β1 reverse allergen-induced airway hyperreactivity and inflammation. J. Clin. Invest. 11, 89–96 (2000).
McWilliam, A.S. et al. Dendritic cells are recruited into the airway epithelium during the inflammatory response to a broad spectrum of stimuli. J. Exp. Med. 184, 2429–2432 (1996).
Akbari, O., DeKruyff, R.H. & Umetsu, D.T. Pulmonary dendritic cells secreting IL-10 mediate T cell tolerance induced by respiratory exposure to antigen. Nature Immunol. 2, 725–731 (2001).
Tsitoura, D.C., Yeung, V.P., DeKruyff, R.H. & Umetsu, D.T. Critical role of B cells in the development of T cell tolerance to aeroallergens. Int. Immunol. 14, 513–523 (2002).
Akbari, O. et al. Antigen-specific regulatory T cells develop via the ICOS-ICOS-ligand pathway and inhibit allergen-induced airway hyperreactivity. Nature Med. (in the press, 2002).
McAdam, A.J. et al. ICOS is critical for CD40-mediated antibody class switching. Nature 409, 102–105 (2001).
Nakajima, A. et al. Requirement of CD28-CD86 co-stimulation in the interaction between antigen-primed T helper type 2 and B cells. Int. Immunol. 9, 637–644 (1997).
Groux, H. et al. A CD4+ T-cell subset inhibits antigen-specific T-cell responses and prevents colitis. Nature 389, 737–742 (1997).
Barrat, F.J. et al. In vitro generation of interleukin 10-producing regulatory CD4+ T cells is induced by immunosuppressive drugs and inhibited by T helper type 1 (Th1)- and Th2-inducing cytokines. J. Exp. Med. 195, 603–616 (2002).
Jonuleit, H. et al. Identification and functional characterization of human CD4+CD25+ T cells with regulatory properties isolated from peripheral blood. J. Exp. Med. 193, 1285–1294 (2001).
Huang, F.P. et al. A discrete subpopulation of dendritic cells transports apoptotic intestinal epithelial cells to T cell areas of mesenteric lymph nodes. J. Exp. Med. 191, 435–444 (2000).
Sauter, B. et al. Consequences of cell death: exposure to necrotic tumor cells, but not primary tissue cells or apoptotic cells, induces the maturation of immunostimulatory dendritic cells. J. Exp. Med. 191, 423–434 (2000).
Sakaguchi, S., Sakaguchi, N., Asano, M., Itoh, M. & Toda, M. Immunologic self-tolerance maintained by activated T cells expressing IL-2 receptor α-chains (CD25). J. Immunol. 160, 1151–1164 (1995).
Thornton, A. & Shevach, E.M. CD4+CD25+ immunoregulatory T cells suppress polyclonal T cell activation in vitro by inhibiting interleukin 2 production. J. Exp. Med. 188, 287–296 (1998).
Tivol, E.A. et al. Loss of CTLA-4 leads to massive lymphoproliferation and fatal multi-organ tissue destruction, revealing a critical negative regulatory role of CTLA-4. Immunity 3, 541–547 (1995).
Zuany-Amorim C et al. Suppression of airway eosinophilia by killed Mycobacterium vaccae-induced allergen-specific regulatory T-cells. Nature Med. 8, 8625–8629 (2002).
Weiner, H.L. The mucosal milieu creates tolerogenic dendritic cells and Tr1 and Th3 regulatory cells. Nature Immunol. 2, 671–672 (2001).
Coffman, R.L., Varkila, K., Scott, P. & Chatelain, R. Role of cytokines in the differentiation of CD4+ T-cell subsets in vivo. Immunol. Rev. 123, 189–207 (1991).
Makela, M.J. et al. IL-10 is necessary for the expression of airway hyperresponsiveness but not pulmonary inflammation after allergic sensitization. Proc. Natl. Acad. Sci. USA 97, 6007–6012 (2000).
Levings, M.K. & Roncarolo, M.G. T-regulatory 1 cells: a novel subset of CD4 T cells with immunoregulatory properties. J. Allergy Clin. Immunol. 106, (Suppl. S) 109–112 (2000).
Akdis, C.A., Blesken, T., Akdis, M., Wuthrich, B. & Blaser, K. Role of interleukin 10 in specific immunotherapy. J. Clin. Invest. 102, 98–106 (1998).
Oh, J.W. et al. CD4 T helper cells engineered to produce IL-10 reverse allergen-induced airway hyperreactivity and inflammation. J. Allergy Clin. Immunol. (in the press, 2002).
Hutloff, A. et al. ICOS is an inducible T-cell co-stimulator structurally and functionally related to CD28. Nature 397, 263–266 (1999).
Aicher, A. et al. Characterization of human inducible costimulator ligand expression and function. J. Immunol. 164, 4689–4696 (2000).
Mages, H.W. et al. Molecular cloning and characterization of murine ICOS and identification of B7h as ICOS ligand. Eur. J. Immunol. 30, 1040–1047 (2000).
Swallow, M.M., Wallin, J.J. & Sha, W.C. B7h, a novel costimulatory homolog of B7. 1 and B7. 2, is induced by TNFα. Immunity 11, 423–432 (1999).
Gonzalo, J.A. et al. ICOS is critical for T helper cell-mediated lung mucosal inflammatory responses. Nature Immunol. 2, 597–604 (2001).
Coyle, A.J. et al. The CD28-related molecule ICOS is required for effective T cell-dependent immune responses. Immunity 13, 95–105 (2000).
Dong, C. et al. ICOS co-stimulatory receptor is essential for T-cell activation and function. Nature 409, 97–101 (2001).
Rottman, J.B. et al. The costimulatory molecule ICOS plays an important role in the immunopathogenesis of EAE. Nature Immunol. 2, 605–611 (2001).
Umetsu, D.T. & DeKruyff, R.H. Th1 and Th2 CD4+ cells in human allergic diseases. J. Allergy Clin. Immunol. 100, 1–6 (1997).
Haneda, K. et al. TGF-β induced by oral tolerance ameliorates experimental tracheal eosinophilia. J. Immunol. 159, 4484–4490 (1997).
Russo, M. et al. Suppression of asthma-like responses in different mouse strains by oral tolerance. Am. J. Respir. Cell. Mol. Biol. 24, 518–526 (2001).
Gerosa, F. et al. Interleukin-12 primes human CD4 and CD8 T cell clones for high production of both interferon-γ and interleukin-10. J. Exp. Med. 183, 2559–2569 (1996).
Tsitoura, D.C. et al. Respiratory infection with influenza A virus interferes with the induction of tolerance to aeroallergens. J. Immunol. 165, 3484–3491 (2000).
Hurst, S.D., Seymour, B.W., Muchamuel, T., Kurup, V.P. & Coffman, R.L. Modulation of inhaled antigen-induced IgE tolerance by ongoing Th2 responses in the lung. J. Immunol. 166, 4922–4930 (2001).
Wannemuehler, M.J., Kiyono, H., Babb, J.L., Michalek, S.M. & McGhee, J.R. Lipopolysaccharide (LPS) regulation of the immune response: LPS converts germfree mice to sensitivity to oral tolerance induction. J. Immunol. 129, 959–965 (1982).
Sudo, N. et al. The requirement of intestinal bacterial flora for the development of an IgE production system fully susceptible to oral tolerance induction. J. Immunol. 159, 1739–1745 (1997).
Ogura, Y. et al. Nod2, a Nod1/Apaf-1 family member that is restricted to monocytes and activates NF-κB. J. Biol. Chem. 276, 4812–4818 (2001).
Ogura, Y. et al. A frameshift mutation in NOD2 associated with susceptibility to Crohn's disease. Nature 411, 603–606 (2001).
Hugot, J.P. et al. Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn's disease. Nature 411, 599–603 (2001).
Neish, A.S. et al. Prokaryotic regulation of epithelial responses by inhibition of IκBα ubiquitination. Science 289, 1560–1563 (2000).
Mahanty, S. et al. High levels of spontaneous and parasite antigen-driven interleukin-10 production are associated with antigen-specific hyporesponsiveness in human lymphatic filariasis. J. Infect. Dis. 173, 769–773 (1996).
Yazdanbakhsh, M., Kremsner, P.G. & van Ree, R. Allergy, parasites, and the hygiene hypothesis. Science 296, 490–494 (2002).
Diez-Gonzalez, F., Callaway, T.R., Kizoulis, M.G. & Russell, J.B. Grain feeding and the dissemination of acid-resistant Escherichia coli from cattle. Science 281, 1666–1668 (1998).
Passalacqua, G. et al. Clinical and immunologic effects of a rush sublingual immunotherapy to Parietaria species: A double-blind, placebo-controlled trial. J. Allergy Clin. Immunol. 104, 964–968 (1999).
Moller, C. et al. Pollen immunotherapy reduces the development of asthma in children with seasonal rhinoconjunctivitis (the PAT-study). J. Allergy Clin. Immunol. 109, 251–256 (2002).
Secrist, H., Chelen, C.J., Wen, Y., Marshall, J.D. & Umetsu, D.T. Allergen immunotherapy decreases interleukin 4 production in CD4+ T cells from allergic individuals. J. Exp. Med. 178, 2123–2130 (1993).
Durham, S.R. et al. Long-term clinical efficacy of grass-pollen immunotherapy. New Engl. J. Med. 341, 468–475 (1999).
Tighe, H. et al. Conjugation of immunostimulatory DNA to the short ragweed allergen amb a 1 enhances its immunogenicity and reduces its allergenicity. J. Allergy Clin. Immunol. 106, 124–134 (2000).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Umetsu, D., McIntire, J., Akbari, O. et al. Asthma: an epidemic of dysregulated immunity. Nat Immunol 3, 715–720 (2002). https://doi.org/10.1038/ni0802-715
Issue Date:
DOI: https://doi.org/10.1038/ni0802-715